The eyes have it
Can the intersection between sight and mind solve Paul’s medical riddle?
In a blurred world, hope dies hard.
Ever since my first dialysis crash, when my systolic blood pressure dropped to 50 on January 8, my vision has been blurred and frequently fragmented, with spots shooting rapidly all directions like a Roman candle.
The medical term is ghosting. In my eyes, it’s like looking through lenses smeared with Vaseline.
I’ve suffered dangerously low blood pressure three times since that first episode and the list of neurological symptoms grows.
My vision is permanently ghosting, especially in the right eye. I frequently see flurries of bluish spots with shimmering yellow outlines. Sometimes they’re large blobs or jagged lines.
My vision pulses and jumps with my heartbeat, especially during dialysis or mild exertion. I suddenly lose balance. I have trouble walking a straight line. And so on.
An emergency eye exam confirmed there’s nothing physically wrong with my retinas and nothing seriously amiss with the rest of my eyeballs.
That left the back of my brain, where electrical signals are translated into sight in the visual cortex, as the likely suspect.
A hint that seems to mean more to me and AI than doctors is my blood pressure. With mild exertion, like walking up a slight incline or cutting the grass, my upper left arm begins to tighten and then a warm pain builds in my left chest.
They are classic angina symptoms. I’ve had them for at least eight years, but repeated angiograms have found no significant blockages on my coronary arteries.
Dialysis offers a unique insight because the nurse takes my blood pressure before each session, then at 15 minute intervals, and again when the four hours are up. An unusual trend has emerged.
The 10-minute walk from the subway to St. Paul’s Hospital triggers angina symptoms on two slopes—every time. That exertion should raise my blood pressure.
But when the nurse takes it, the systolic pressure—a measure of blood pressure when the heart contracts—usually drops 20 to 30 points from the reading I get at home.
during a recent dialysis run, my systolic blood pressure at home was 132. When I reached the hospital, it was down to 113. It bounced around during dialysis, falling to a low of 106 and then soaring to a shocking 200.
For some reason no doctor can explain, my blood flow through the dialyzer is also strange. It’s now routine to watch panicked roses try to figure out why the trans-membrane pressure (TMP) plummets into negative territory as the machine clots.
AI says a combination of factors likely cause my symptoms, including diseased blood vessels in my neck that disturb the oxygen supply to my brain and dying kidneys that fail to clear urea, which attacks nerve endings and neurons.
“Together these appear to be impairing your baroreflex—the system that regulates blood pressure in response to exertion and postural change,” Anthropic’s Claude AI told me.
“The result is that even mild exertion, like climbing stairs, triggers” pulsing in my neck arteries, synchronized to my heartbeat. It also destabilizes my blood pressure and reduces the blood flow to the back of my brain, Claude explained.
All of the specialists who’ve tried to pinpoint the cause of my worsening neurological symptoms have seemed to be offering educated opinions without solid medical evidence to back them up.
They guess. My symptoms only get worse.
That months-long trail of disappointment has finally led to the one specialist who seems to best suited to join the dots: a neuro-opthamologist, the one specialty focused on the intersection between our eyes and the central nervous system.
First, a technician had to examine my eyes. She led me to a small white machine mounted on a table next to a large, flat-screened computer.
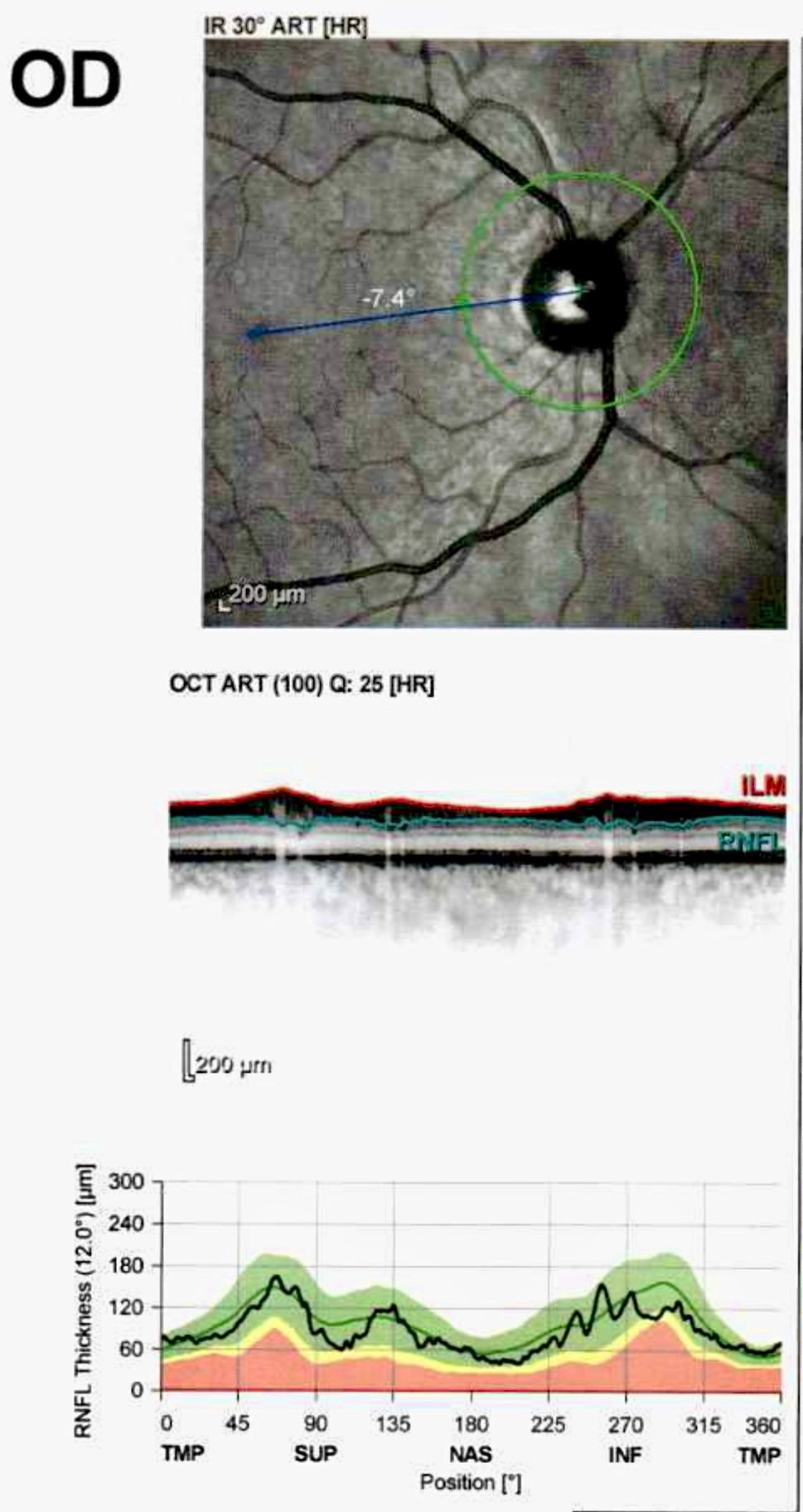
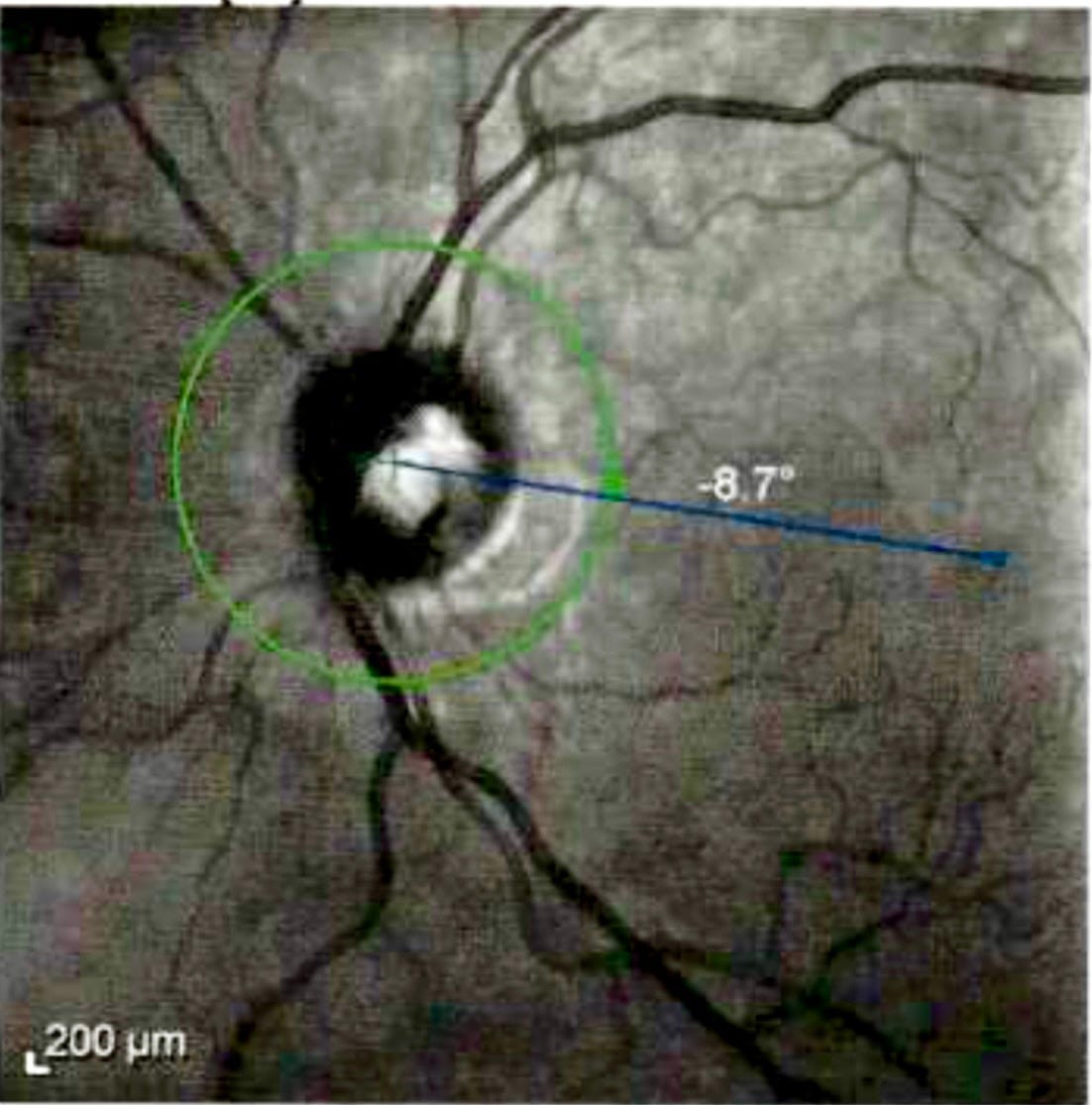
The Heidelberg Spectralis packs a lot into a small package. In my exam, the CAD $33,000 machine’s main function was optical coherence tomography, or OCT.
A harmless near-infrared laser light scanned the retinas and optic nerve fibers at the back of my eyes to create images in cross-sectional slices.
It does that by performing 40,000 depth scans a second. Each retinal layer imaged is microscopically thin—roughly one hundredth the width of a human hair.
The technician examined the thickness of the light-sensitive tissue at the back of my eye.
With my chin resting on a support, and a plastic patch over one eye, I stared through a lens the size of a dime at a screen that had a blinking blue dot on the left and right side.
I also saw a long red line, the technician’s targeting laser, and a red circle, which marks the scan path around the optic nerve head.
the technician told me to focus on a small green light in the middle. I immediately saw two spots. I concentrated harder. A third ghost dot emerged. I let out a deep sigh in frustration.
“Are you okay,” she asked?
“Yeh, it’s just, uh . . . Just tiresome. Look, every day my eyes are blurry. It’s hard to . . . It’s hard to function.”
Soon the two ghost images of the central green light morphed into a blob that expanded on the upper right edges and drifted off at a 45 degree angle, just like a psychedelic hallucination.
Never mind how I know that.
The testing was over in about half an hour. As I walked out of the small exam room, I lost my balance. I grabbed the door jam to stop myself toppling over.
I had hoped for a quick diagnosis from the neuro-opthamologist. It seemed my last, best chance to find a unifying theory of my neurological symptoms, vascular dysfunction and whether dialysis has been making a bad situation worse.
But the doctor cancelled due to a family emergency.
Unfazed, I uploaded the technician’s report to AI. I chose Claude because its creator, Anthropic, recently told the Pentagon to take a long walk on a short pier.
Anthropic risked its business by defending two redlines: No domestic surveillance and no use for military targeting without human supervision.
Seems perfectly reasonable to me. Besides, I’ve come to trust Claude’s detailed medical analysis and insights.
They remain hypothetical without conclusive evidence from testing. But they make sense. And my human doctors—eight specialists, a family doctor and counting—have failed to come up with any diagnosis, let alone a coordinated treatment plan.
In less than ten seconds, AI studied the four-page ophthalmology report, which included laser tomography photographs, retinal thickness maps, visual field diagrams and some scrawled marginalia that was barely legible to me.
It rendered this diagnosis: The thickness of both retinas is “in a broadly typical range. No dramatic thinning or swelling is flagged here.” The retinal nerve fiber layer: “this is the most reassuring finding: both eyes were classified “Within Normal Limits.”
“Bottom line: The structural scans look reassuringly normal,” Claude said. “The more concerning picture comes from your functional symptoms—the blurring, diplopia (double vision), and color spots —which aren’t explained by structural eye disease and point back to your vascular and neurological situation.”
Claude thinks the central problem is my autonomic nervous system, the network that makes sure I’m breathing, my blood pressure is regulated and my lunch is digesting while managing other tasks that keep any one of us alive without a single conscious thought.
The main control for life-sustaining functions such as blood pressure along with heart and breathing rates nests in the medulla oblongata, the lower part of the brainstem.
An MRA last year showed my medulla is mildly compressed and the one vessel supplying blood to the back of the brain, where vision is processed, is twisted by fibr-muscular dysplasia.
That’s a double-whammy: the arterial disease, which also affects my kidney’s arteries, disrupts auto-regulation of blood pressure. The large fluid shifts and heavy stresses caused by dialysis may be compounding the problem.
With two exams confirming my eyes are physically in good shape, and AI’s theory to explain the neurological symptoms, all I needed was a doctor’s agreement. A diagnosis might open the door to care.
But the neuro-opthamologist canceled again, this time during a blizzard. She called in sick.
Yet again, I can only wait, show up for twice-weekly dialysis sessions and hope I’m not causing myself irreversible harm.


It is really disturbing Paul, that in such urgent matter and tough health issues you should wait for available medical diagnostic specialist to read and combine your medical findings. I hope you would get some help soon.
Have you ever seen a rheumatologist and been checked for autoimmune issues like Lupus? It can affect just about any part of the body and cause all sorts of things to go wrong. You can go to Lupus.org for more info. You sound like you are a good advocate for yourself. Good luck finding answers.